Platelet (PlA1/A2) and Nitric Oxide Synthase Gene Polymorphisms (Glu298Asp, -786T>C, 922A/G and Intron 420/393) and Its Relation with In-Stent Restenosis
pp. 471-477
DOI:
https://doi.org/10.7775/rac.v77i6.2200Keywords:
Genetics, Coronary Stenosis, PolymorphismAbstract
Background
The advent and the development of drug eluting stents (DES) have reduced the prevalence of restenosis according to different series; however, its incidence still remains significant. Genetic factors contribute to restenosis and thus should be taken into account and undergo thorough investigation. Some polymorphisms are known to have a relation with in-stent restenosis: platelet polymorphism and endothelial nitric oxide synthase gene polymorphism.
Objective
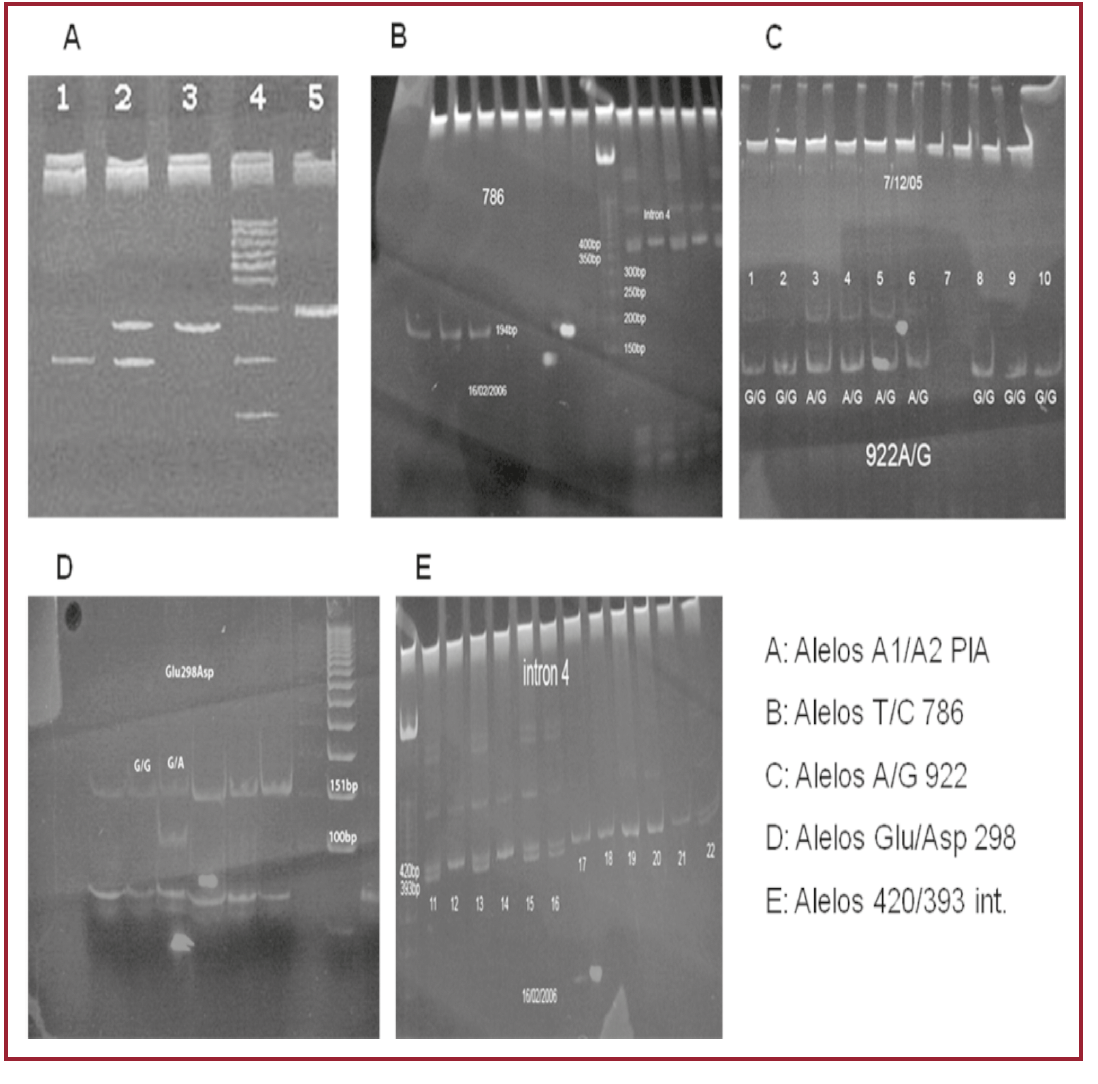
To demonstrate if platelet IIb-IIIa (PlA2) and endothelial nitric oxide synthase (eNOS) gene polymorphisms (Glu298Asp, -786T>C, 922A/G and 420/393) present greater risk of in-stent restenosis after coronary angioplasty (PTCA).
Material and Methods
A coronary angiography was performed in 92 patients who had undergone PTCA in the previous 1 to 12 month, due to suspected restenosis. Patients were divided in two groups: with angiographic restenosis (<50%) (cases) and without restenosis (controls). A polymerase chain reaction (PCR) was performed for each polymorphism using specific restriction enzymes. Multiple logistic regression analysis included clinical, angiographic and genetic factors.
Results
Age, gender and risk factors were similar among both groups (cases = 41 patients with restenosis, controls: 51 patients without restenosis). A 60% of drugs eluting stents were implanted in each group. The rate of restenosis in patients with PlA2 polymorphic allele was significantly greater than in non carriers (21.9% versus 1.9%, OR 14.1, 95% CI 1.7-116.3; p=0.002). Patients with variant allele for 922A/G polymorphism showed a similar behavior (41.5% versus 19.6%, OR 2.9, 95% CI 1.2-7.4; p=0.02). The prevalence of restenosis was similar in both groups in patients with 298Asp, 420/393 and 786T-C polymorphisms. Multivariate analysis revealed that PlA1/A2 was the only predictor of restenosis (p=0.02).
Conclusions
This study demonstrates that PlA2 polymorphic allele is an independent predictor of in-stent restenosis; its detection might have important clinical implications in decisionmaking.
Downloads
Published
Issue
Section
License
Copyright (c) 2025 Argentine Journal of Cardiology

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.













