Antioxidant Role of Vitamin E in Atherogenesis induced by Hyperfibrinogenemia
pp 405-410
DOI:
https://doi.org/10.7775/rac.v78i5.1943Keywords:
Hyperfibrinogenemia, Atherogenesis, Oxidative stress, Superoxide dismutase, Vitamin EAbstract
We used an experimental model of atherogenesis to evaluate the effect of vitamin E on oxidative stress induced by hyperfi-
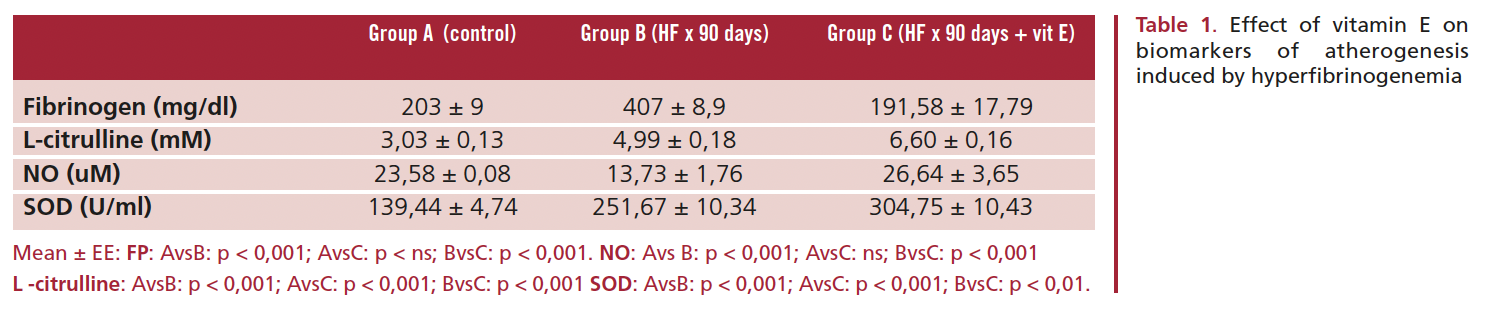
brinogenemia (HF) and the possible normalization of oxidative stress markers. The following variables were studied: nitric oxide (NO), L-citrulline, superoxide dismutase (SOD) activity and regression of histopathological lesions in the thoracic aorta. The study was performed in 36 Wistar rats that were divided into three groups of 12 rats each: A, control group; B, HF for 90 days; C, HF for 90 days + vitamin E. Hyperfibrinogenemia was induced by the injection of epinephrine (0.1 ml/day/rat) during 90 days. The dose of vitamin E was 2 mg/day/rat during 75 days. We measured the plasma levels of fibrinogen (mg/dl), NO (uM) and L-citrulline (mM); SOD activity (U/ml) was assayed in red cell lysates using spectrophotometry. The histopathological sections of the thoracic aorta were examined using light micros- copy (LM). Statistical analysis was performed using MANOVA and Fisher’s test; a p value <0.05 was considered statistically significant. Rats in group B had a significant increase in fibrinogen levels B (407±8.9 mg/dl) compared to groups A (203±9 mg/dl) and C (191.58±17.79 mg/dl) (p<0.001). We observed a significant decrease in NO in group B (13.73±1.76 uM) versus groups A (23.58±0.08 uM) and C (26.64±3.65 uM) (p<0.001). L-citrulline increased significantly in groups B (4.99±0.18 mM) and C (6.60±0.16 mM) compared to group A (3.03±0.13 mM) (p<0.001). SOD activity was greater in groups B (251.67±10.34 U/ml) and C (304.75±10.43 U/ml) versus group A (139.44±4.74 U/ml) (p<0.001). Light microscopic examination revealed the presence of endothelial denudation, intimal thickening and vessel wall protrusion in group B (90%), while recovery of endothelial denudation and a 50% reduction in intimal thickening was observed in group C (p<0.001). High SOD activity might be insufficient to prevent abnormalities in the oxidative stress pathway induced by HF. Vitamin E would stop the chain reaction initiated by free radicals and thus decrease the superoxide anion, stimulating the bioavailability of NO with normalization of fibrinogen plasma levels.
Downloads
Published
Issue
Section
License
Copyright (c) 2025 Argentine Journal of Cardiology

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.












