Impact of Cusp-Overlap Technique on Pacemaker Requirement after Transcatheter Aortic Valve Implantation
pp 136-139
DOI:
https://doi.org/10.7775/rac.es.v89.i2.19091Keywords:
Transcatheter aortic valve replacement, Atrioventricular block, Pacemaker, Artificial, Heart Valve Prosthesis Implantation, methodsAbstract
Background: Persistent bradyarrhythmias requiring permanent pacemaker implantation are a common complication after transcatheter aortic valve implantation (TAVI), but high implantation with cusp-overlap technique could prevent conduction system disturbances.
Objective: The aim of this study was to assess the rate of pacemaker use in patients who received TAVI with conventional coplanar technique compared with cusp overlap technique.
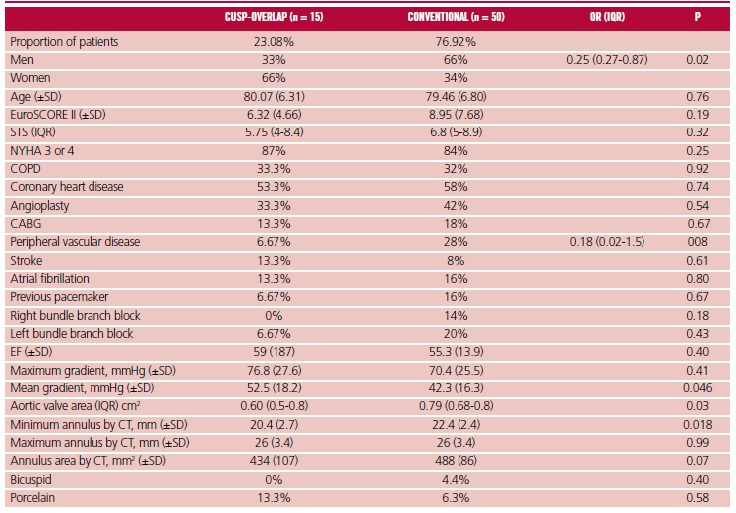
Methods: A total of 65 consecutive patients from two centers receiving Evolut-R or Evolut-Pro valve implantation, 50 coplanar and 15 cusp-overlap, were analyzed between 2017 and 2019.
Results: Mean age was 80 years, and there were no differences in risk according to the EuroSCORE. The rate of pacemaker requirement was 0% in cusp-overlap procedures compared with 24.9% in those with conventional implantation (OR=0.0; 95% CI 0-0.89; p=0.041). In addition, cusp-overlap implants presented lower rate of major complications (6.67% vs. 42%; OR=0.09; 95% CI 0.01-0.8; p=0.011).
Conclusions: In this cohort, TAVI procedure with cusp-overlap technique was associated with null pacemaker requirement. Given the potential large-scale impact, external validation of results is needed.
Downloads
Published
Issue
Section
License
Copyright (c) 2021 Argentine Journal of Cardiology

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.













